Great Ormond Street Hospital (GOSH) recently used a pioneering treatment to transplant otherwise-discarded thymus tissue into very young children who lack a working thymus.
Your thymus gland plays a crucial role in the production of your T-cells, which are white blood cells that are essential for fighting infections. Infants born without a thymus are “athymic”, frequently as a result of complete DiGeorge syndrome (cDGS). This rare disorder leaves infants at a high risk of becoming extremely ill. If an infection is encountered and the athymia is not treated within the first 2 years of life they are likely to die.
Luckily, a procedure to resolve athymia has been developed- a thymus transplant. This requires the transplant of healthy thymus tissue from one individual, which is then grown in the laboratory, into the thigh muscle of the recipient patient.
The thymus tissue is usually obtained from children with congenital heart disease undergoing surgery, with parental consent, since thymus tissue is removed to gain access to the heart. It would otherwise be discarded, so this is at no detriment to the donor and has minimal risk since their immune system is already developed and not all of the gland is usually removed.
Current data shows that approximately 75 percent of patients with cDGS have a successful outcome from a thymus transplant. After the procedure, patients are seen to develop T-cells, allowing them to fight the most common infections, come off preventative measures such as antibiotics, and are able to attend nursery and school.
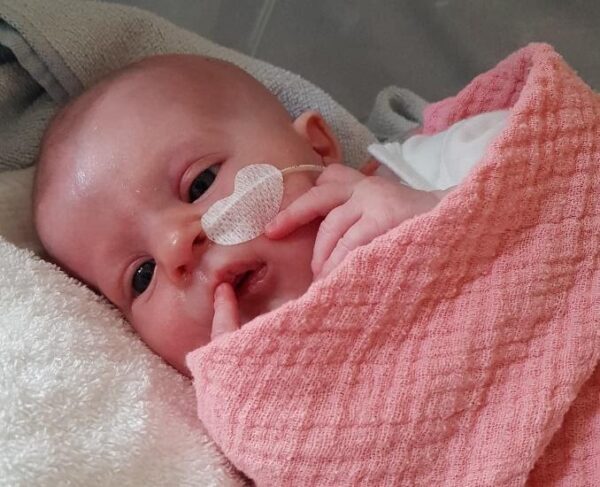
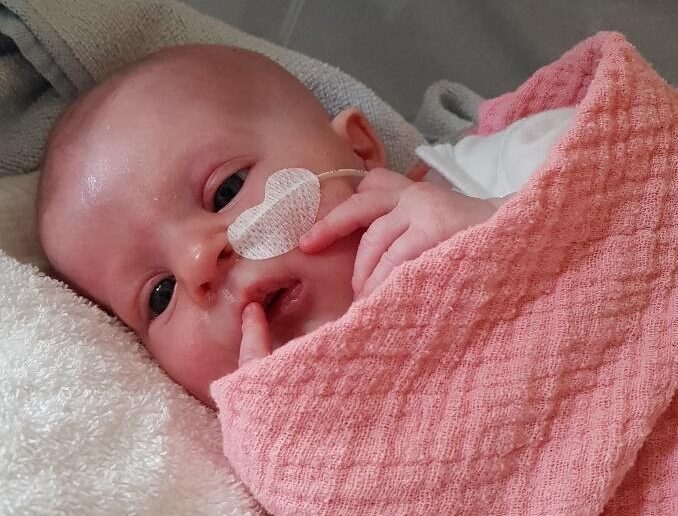
Four-month-old Florentina from Gatringen, Germany, became the 50th patient at GOSH to receive this life-saving procedure. Since GOSH is one of only two centres in the world to carry out this procedure – the other being Duke University in the USA – the hospital receives patients from all across the globe, even from as far as New Zealand!

Florentina’s transplant was deemed successful, although it is too early to know the long-lasting positive effects. Regardless, the doctors are pleased with Florentina’s progress so far and there have been several other positives of Florentina’s trip to GOSH.
Since Florentina is highly susceptible to infection, her mother Stefanie has had to wear a face mask whilst interacting with her since her birth. Stefanie explained, “Until we arrived at GOSH, she hadn’t seen me without a mask. This is the first time she’s seeing anyone, including myself without one. I love how I can now properly converse with her.”
Due to the COVID-19 pandemic, the transplantation programme was suspended in March 2020 as the team were required for COVID-related clinical duties. However, to reduce the risk of severe complications as a result of the growing waiting list, the programme was granted special permission from NHS England to resume accepting patients. This was clearly the right choice, as in 2020, GOSH treated 10 patients. This is double the average number performed in each other previous three years.
Some patients can develop complications after transplantation as a result of the new T-cells being poorly regulated which can cause some damage to the body’s own tissues. These problems are usually treatable, but the research team, based at the Zayed Centre for Research into Rare Disease in Children at GOSH are working to optimise the process and reduce the chance of such complications.
This £1million programme is funded by Great Ormand Street Hospital Children’s Charity (GOSH Charity) and provides the support needed for researchers and clinicians at the hospital to further develop this treatment to reduce the chances of post-operative complications. Dr Kiki Syrad, Director of Grants and Impact at GOSH Charity, said: “It is fantastic that 50 children have now benefited from this pioneering technique with many more to be helped in the future […] This is exactly the kind of life-changing impact that funding for paediatric research can offer to seriously ill children and their families, and is why funding research remains so important.”